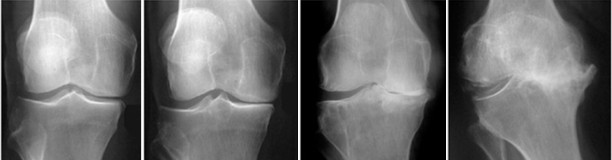
Arthrosis / Knee arthroplasty
Arthrosis is defined as a degenerative condition characterized by the wearing of the cartilage covering the bone ends in a joint. Articular movements are enabled by the sliding of cartilaginous surfaces at the femur’s lower end, the tibia’s upper end, and the posterior side of the patella.
Over time and with use, cartilage thickness decreases, and its surface gets uneven, leading to painful movements. X-rays show a narrowed joint space whose extent depends on the severity of osteoarthritis. When the cartilage is completely worn out, articular contact is made between the bones, causing a lot of pain. In this event, X-rays show that the narrowed joint space has vanished, and sometimes reveal bone wear and osseous outgrowths called “osteophytes” as well. Osteoarthritis often arises in conjunction with degenerescence and meniscal lesions.
L’arthrose est le plus souvent associée à une dégénérescence puis à des lésions méniscales.
Main causes of cartilage wear:
- Osteoarthritis: Osteoarthritis of the knee (gonarthrosis) may be caused by overweight, joint fracture after-effects, inward (varus) or outward (valgus) lower limb misalignment, old cruciate ligament ruptures, and meniscus removal;
- Rheumatoid arthritis or other inflammatory rheumatisms;
- Osteonecrosis, involving mostly the femur.
The best surgical option is set according to the extent of cartilage wear, the patient’s age, and the type of osteoarthritis.
- Cartilage graft
- Osteotomy
- Knee prostheses