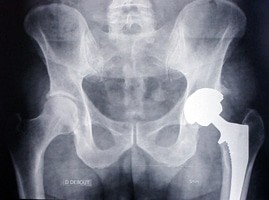
Total hip replacement
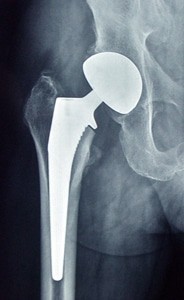
This surgery is conducted when the cartilage covering the femoral head and the inside of the cotyla wears out.
A hip prosthesis includes
- A long part, made of titanium, firmly secured into the femur (femoral cask),
- on which we mount a sphere (the femoral head), usually a ceramic;
- a hollow cup made of titanium or steel and firmly secured into the cotyla, in which we insert a polyethylene or ceramic cup that ensures friction with the femoral head;
- an additional element can be placed between the polyethylene and the acetabular cup, which is called dual mobility cup.
Primary fixation is ensured by impacting the prosthesis into the bone. The stability of this initial fixation is called “primary stability.” Preparation for this step should be done carefully. The cotyla is prepared with drills of increasing diameter, and the prosthetic acetabular hemisphere is firmly secured into it. The femur is prepared with reamers of increasing size, which are shaped like the prosthesis. The femoral part is then secured into this cavity. Prosthetic parts are 1mm to 1.5mm larger than drills and reamers in order to guarantee primary stability. They are covered with hydroxapatite, one of bone’s mineral components. It facilitates bone regrowth and adhesion to the prosthesis, ensuring permanent stability ( “secondary stability”).
The decision to undergo surgery belongs to the patient, who should take into consideration his functional discomfort (pain, mobility loss, as well as the intake of analgesics and anti-inflammatory medication).
The procedure usually lasts about 1.5 hours.
Hip replacement surgery is considered depending on the patient’s age-ideally, older than 60. Before this age, a prosthesis may be required if all other medical treatments, including intra-articular hyaluronic acid injections, have failed.
The younger the patient, the more we prefer medical treatments in order to delay the implantation of this prosthesis. For young patients for whom prosthesis implantation is deemed necessary, we favor “hard-hard” friction couples (ceramic/ceramic or steel/steel) on resurfacing cups.
Unfortunately, complications are always possible during surgery (for example, nervous and vascular damage, including sciatic nerve stretching that could lead to partial paralysis, which usually decreases after 3 months, and bone cracks or femoral cask fractures). Other potential post-surgery complications include phlebitis, pulmonary embolism, and prosthesis dislocation within the first 3 months after surgery. The dislocation risk is greatly decreased and close to zero with double mobility prostheses. Because of this risk, the double mobility prosthesis is the preferred option for elderly patients, with decreased muscle control.
Minimally invasive techniques have been developed since the beginning of 2000’s. I have been using them since 2004. These procedures allow for smaller incisions and better muscle access. The incision is usually 6cm long on normal-sized patients. The use of these techniques results in less painful postoperative recoveries and faster recovery of walking. Crutches are no longer be needed 2 weeks after surgery, but rehabilitation is essential so as to recover proper joint use and muscle control–even more so as there is always muscle deficiency in patients with painful hip osteoarthritis.